17 results
“Acute urinary antibiotics”—A simple metric to identify outpatient antibiotic stewardship opportunities in renal transplant
- Alex Zimmet, David Ha, Emily Mui, Mary Smith, William Alegria, Marisa Holubar
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 3 / Issue S2 / June 2023
- Published online by Cambridge University Press:
- 29 September 2023, pp. s76-s77
-
- Article
-
- You have access Access
- Open access
- Export citation
-
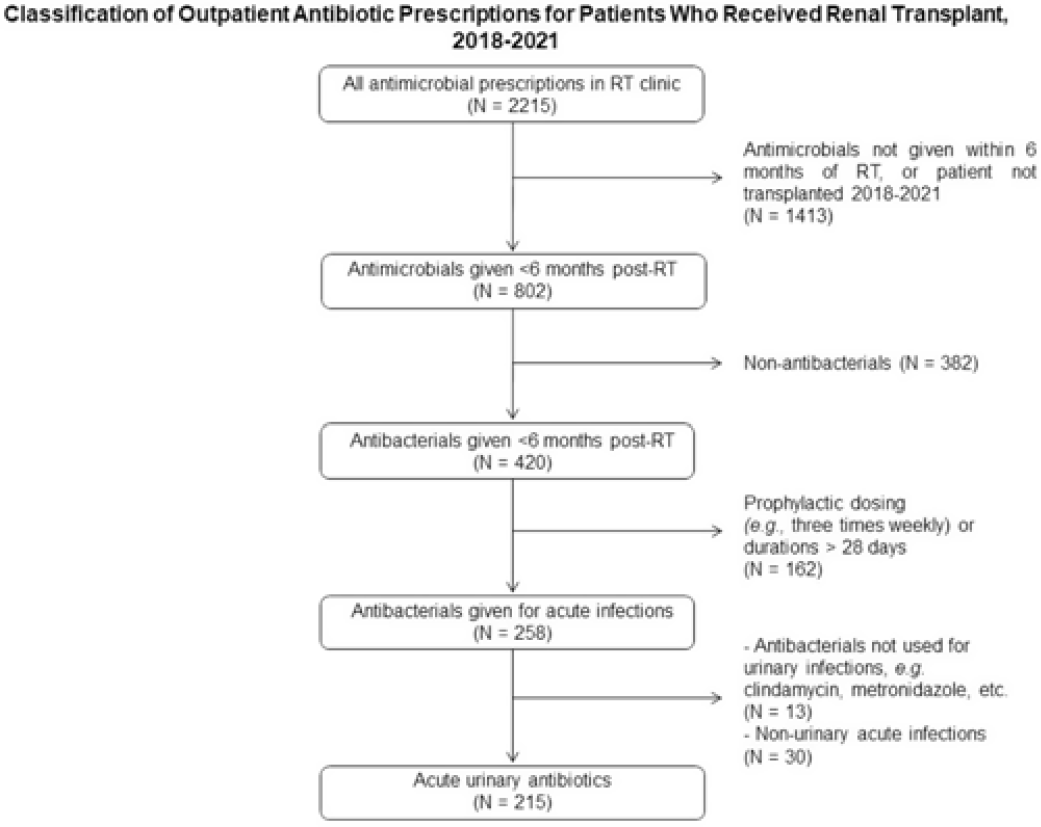
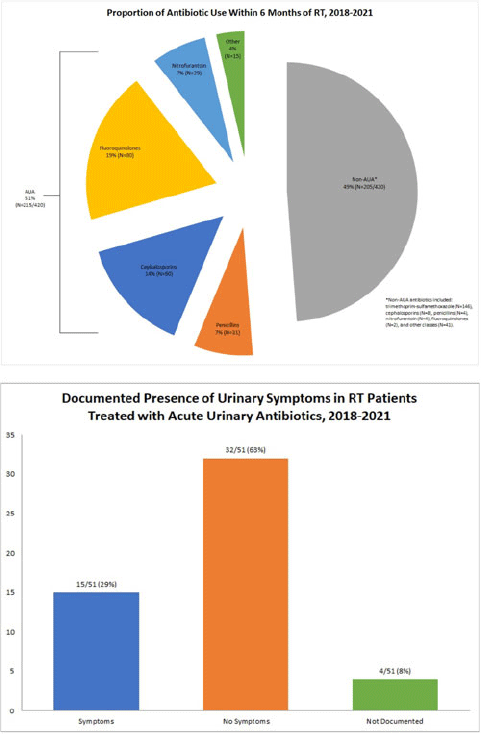
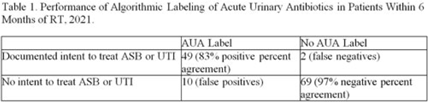
Background: International Classification of Diseases, Tenth Edition (ICD-10) data help track outpatient antibiotic prescribing but lack validation in immunocompromised populations or subspecialty clinics for this purpose. Asymptomatic bacteriuria (ASB) and urinary tract infection (UTI) are important stewardship targets in renal transplant (RT) patients, but they may require alternative metrics to best monitor prescribing patterns. We describe ICD-10 utilization for RT clinic encounters in which antibiotics were prescribed. We developed a metric classifying “acute urinary antibiotics” (AUA) to track antibiotic use for ASB and UTI, and we validated systematic identification of AUA to enable practical implementation. Methods: We examined RT clinic visit and telemedicine encounters from 2018 to 2021 conducted 1 month after transplant. This project was deemed non–human-subjects research by the Stanford Panel on Human Subjects in Medical Research. Results: The analytic cohort included 420 antibacterial prescriptions from 408 encounters (Fig. 1). Of 238 patients, 136 (57%) were male and 112 (47%) were Hispanic or Latino. The most common primary ICD-10 code was Z94.0 (kidney transplant status) (N = 302 of 408 encounters, 75%); 26 encounters (6%) were coded for UTI (eg, N39.0, urinary tract infection, site not specified); and 214 encounters (53%) had multiple ICD-10 codes. The R82.71 code (bacteriuria) was never used. However, 215 prescriptions (51%) were classified as AUA (Fig. 2). The validation cohort included 130 prescriptions; 59 (45%) were classified as AUA and 51 (39%) had documented intent to treat ASB or UTI (positive percent agreement, 83%; negative percent agreement, 97%) (Table 1). For patients >1 month after transplant, the positive percent agreement was 95% and the negative percent agreement was 98%. Of 51 patients receiving AUA, 32 (63%) were asymptomatic despite frequently having a code for UTI (Fig. 3). Conclusions: ICD-10 coding may not be helpful in monitoring antibiotic prescribing in RT patients. The AUA metric offers a practical alternative to track antibiotic prescribing for urinary syndromes and reliably correlates with physician intent. Monitoring AUA prescribing rates could help identify opportunities to optimize antibiotic use in this complex outpatient setting.
Disclosures: None
Electronic phenotyping of community-acquired pneumonia: A tool for inpatient syndrome-specific antimicrobial stewardship
- Amy Chang, Annie Bui, David Ha, William Alegria, Marisa Holubar, Brian Lu, Leah Mische, Rebecca Linfield, Kyle Walding, Emily Mui
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 3 / Issue S2 / June 2023
- Published online by Cambridge University Press:
- 29 September 2023, pp. s114-s115
-
- Article
-
- You have access Access
- Open access
- Export citation
-
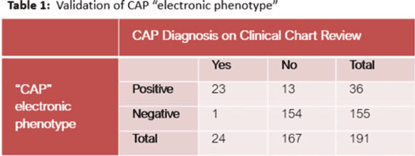
Background: Using patient data from the electronic health record (EHR) and computer logic, an “electronic phenotype” can be created to identify patients with community-acquired pneumonia (CAP) in real time to assist with syndrome-specific antimicrobial stewardship efforts.1 We adapted and validated the performance of an inpatient CAP electronic phenotype for antimicrobial stewardship interventions. Methods: An automated scoring system was created within the EHR (Epic Systems) to identify hospitalized patients with CAP based on the variables and logic listed in Fig. 1B. We adapted a score used by the Michigan Hospital Medicine Safety Consortium (HMS) to identify patients with CAP, with additions made to improve sensitivity (Fig. 1).1 The score can be displayed in a column within the EHR patient list (Fig. 2). We validated the electronic phenotype via chart review of all hospitalized patients on systemic antimicrobials admitted to a medicine team consecutively between November 8 and 18, 2021. Patients who were readmitted within the validation time frame were excluded. We assessed the performance of the electronic phenotype by comparing the score to manual chart review, where “CAP diagnosis” was defined as (1) mention of “pneumonia” or “CAP” as part of the differential diagnosis in the admission documentation, (2) antimicrobials were started within 48 hours of admission, and (3) radiographic findings were suggestive of pneumonia. After initial evaluation, the scoring system was adjusted, and performance was re-evaluated during prospective audit and feedback performed on EHR CAP–positive patients over 13 days between July 2022 and December 2022. Results: We included 191 patients in our initial validation cohort. The CAP score had high sensitivity (95.83%), specificity (92.2%), and negative predictive value (99.35%), though lower positive predictive value (63.89%) was noted (Table 2). The rules were further refined to include bloodstream infection only with Haemophilus influenza or Streptococcus pneumoniae in rule 2B, and azithromycin was removed from “CAP antibiotics.” After these changes, repeated evaluation of 88 patients with positive CAP EHR score was performed, and only 20 (23%) were considered false-positive results. Conclusions: Electronic phenotypes can be used to create automated tools to identify patients with CAP with reasonable performance. Data from this tool can be used to guide more focused antimicrobial stewardship interventions and clinical decision support in the future. Reference: Vaughn VM, et al. A statewide collaborative quality initiative to improve antibiotic duration and outcomes in patients hospitalized with uncomplicated community-acquired pneumonia. Clin Infect Dis 2022;75:460–467.
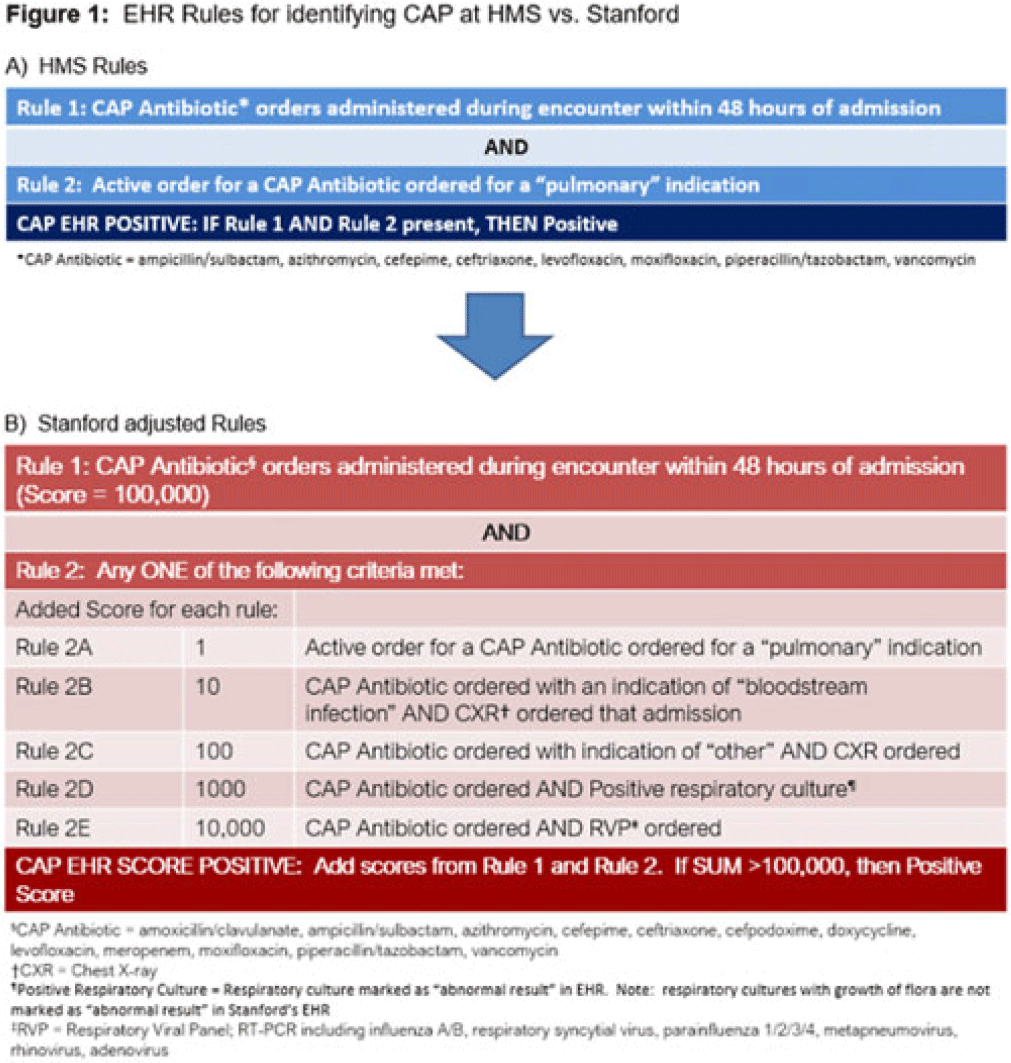
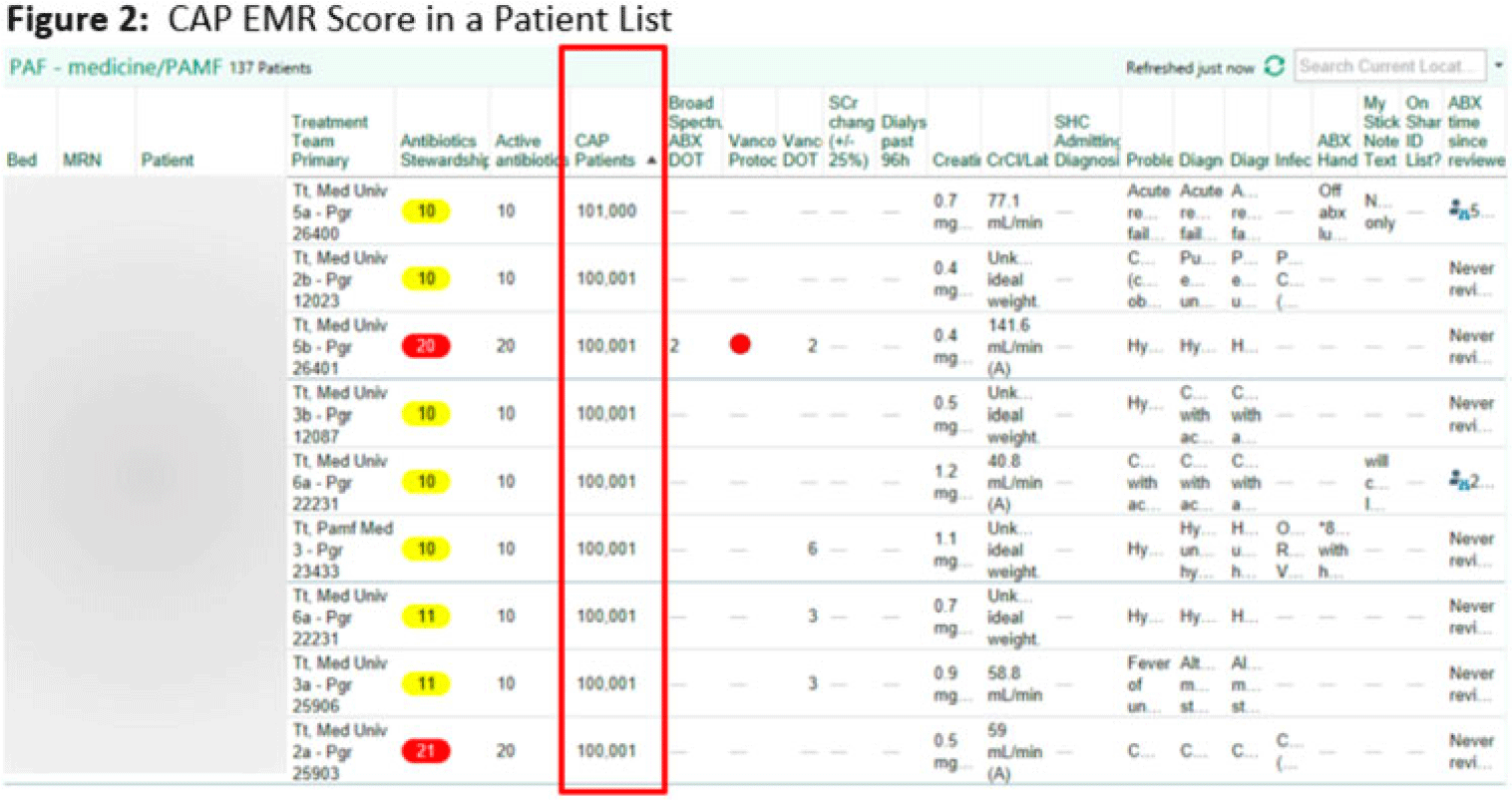
Disclosures: None
A quality-improvement approach to urgent-care antibiotic stewardship for respiratory tract infections during the COVID-19 pandemic: Lessons learned
- Sharon K. Ong’uti, Maja Artandi, Brooke Betts, Yingjie Weng, Manisha Desai, Christopher Lentz, Ian Nelligan, David R. Ha, Marisa K. Holubar
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 44 / Issue 12 / December 2023
- Published online by Cambridge University Press:
- 23 February 2023, pp. 2022-2027
- Print publication:
- December 2023
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
Objective:
We investigated a decrease in antibiotic prescribing for respiratory illnesses in 2 academic urgent-care clinics during the coronavirus disease 2019 (COVID-19) pandemic using semistructured clinician interviews.
Methods:We conducted a quality-improvement project from November 2020 to May 2021. We investigated provider antibiotic decision making using a mixed-methods explanatory design including interviews. We analyzed transcripts using a thematic framework approach to identify emergent themes. Our performance measure was antibiotic prescribing rate (APR) for encounters with respiratory diagnosis billing codes. We extracted billing and prescribing data from the electronic medical record and assessed differences using run charts, p charts and generalized linear regression.
Results:We observed significant reductions in the APR early during the COVID-19 pandemic (relative risk [RR], 0.20; 95% confidence interval [CI], 0.17–0.25), which was maintained over the study period (P < .001). The average APRs were 14% before the COVID-19 pandemic, 4% during the QI project, and 7% after the project. All providers prescribed less antibiotics for respiratory encounters during COVID-19, but only 25% felt their practice had changed. Themes from provider interviews included changing patient expectations and provider approach to respiratory encounters during COVID-19, the impact of increased telemedicine encounters, and the changing epidemiology of non–COVID-19 respiratory infections.
Conclusions:Our findings suggest that the decrease in APR was likely multifactorial. The average APR decreased significantly during the pandemic. Although the APR was slightly higher after the QI project, it did not reach prepandemic levels. Future studies should explore how these factors, including changing patient expectations, can be leveraged to improve urgent-care antibiotic stewardship.
Impact of different COVID-19 encounter definitions on antibiotic prescribing rates in urgent care
- Sharon Onguti, David Ha, Emily Mui, Amy Chang, Eddie Stenehjem, Adam Hersh, Marisa Holubar
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 2 / Issue S1 / July 2022
- Published online by Cambridge University Press:
- 16 May 2022, p. s5
-
- Article
-
- You have access Access
- Open access
- Export citation
-
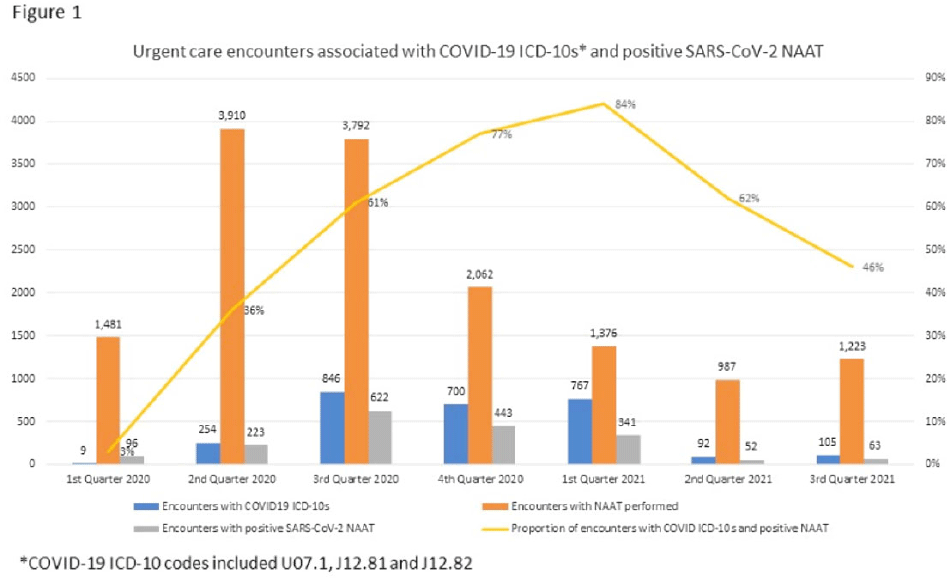
Background: Billing data have been used in the outpatient setting to identify targets for antimicrobial stewardship. However, COVID-19 ICD-10 codes are new, and the validity of using COVID-19 ICD-10 codes to accurately identify COVID-19 encounters is unknown. We investigated COVID-19 ICD-10 utilization in our urgent care clinics during the pandemic and the impact of using different COVID-19 encounter definitions on antibiotic prescribing rates (APRs). Methods: We included all telemedicine and office visits at 2 academic urgent-care clinics from January 2020 to September 2021. We extracted ICD-10 encounter codes and testing data from the electronic medical record. We compared encounters for which COVID-19 ICD-10 codes were present with encounters for which SARS-CoV-2 nucleic acid amplification testing (NAAT) was performed within 5 days of and up to 2 days after the encounter (Fig. 1). We calculated the sensitivity of the use of COVID-19 ICD-10 codes against a positive NAAT. We calculated the APR as the proportion of encounters in which an antibacterial drug was prescribed. This quality improvement project was deemed non–human-subjects research by the Stanford Panel on Human Subjects in Medical Research.
Funding: None
Disclosures: None
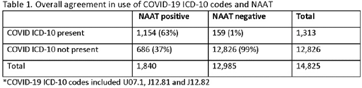
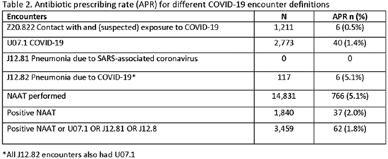
Metrics in outpatient stewardship: Is more always better?
- Natalia Medvedeva, David Ha, Sharon Onguti, Emily Rosen, Emily Mui, Sean Pearce, Alex Schneider, Amy Chang, Adam Hersh, Eddie Stenehjem, Marisa Holubar
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 2 / Issue S1 / July 2022
- Published online by Cambridge University Press:
- 16 May 2022, pp. s70-s71
-
- Article
-
- You have access Access
- Open access
- Export citation
-
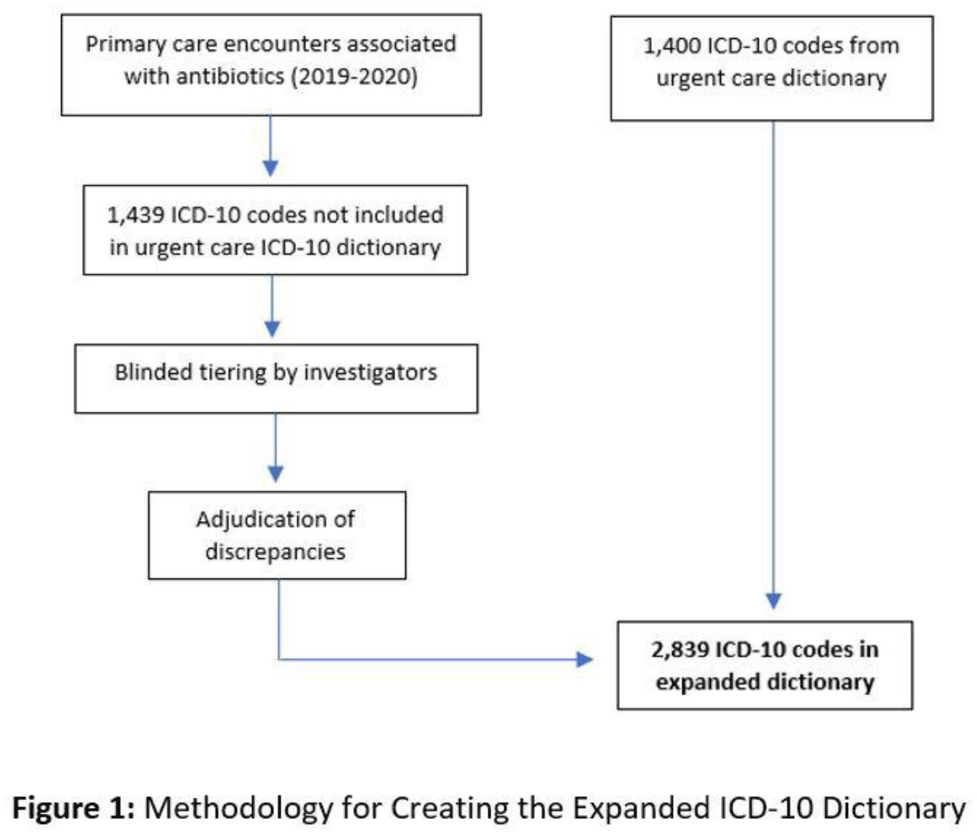
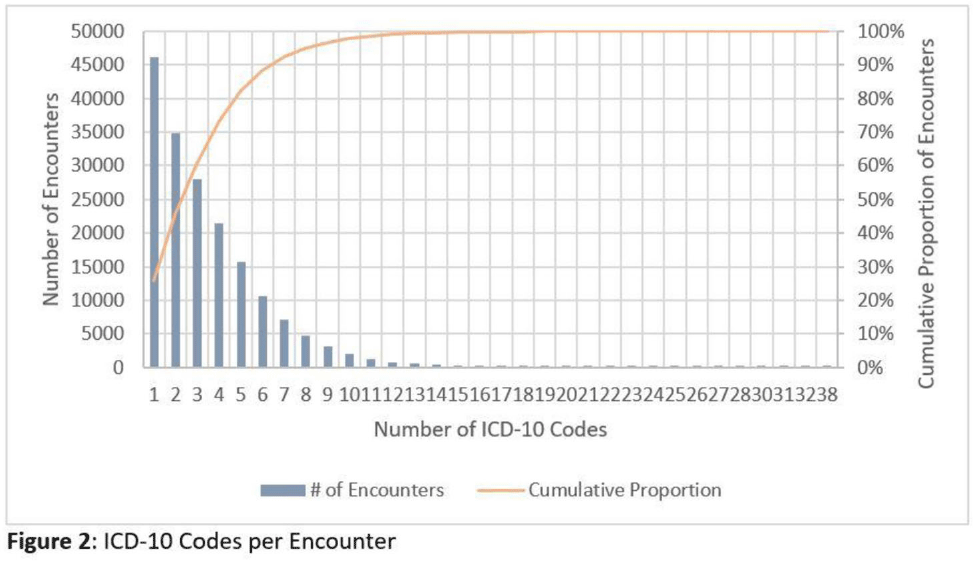
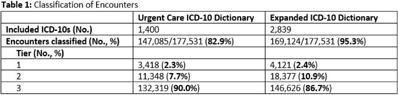
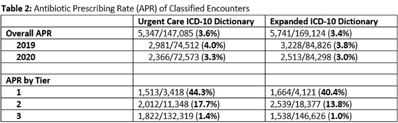
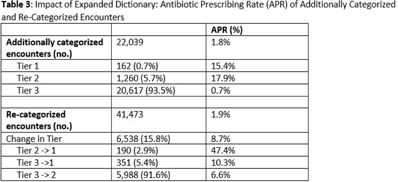
Background: Emerging evidence supports the use of billing data to identify stewardship targets in primary care. Standardizing an approach to antibiotic prescribing rate (APR) calculations could facilitate external benchmarking. Methods: Using methodology and an ICD-10 dictionary validated in urgent care clinics,1 we created an expanded ICD-10 dictionary to incorporate additional ICD-10 codes from primary care associated with antibiotic prescriptions (Fig. 1). We then compared antibiotic prescribing rates using the urgent care and expanded dictionaries. We included all primary care visits from 2019 to 2020 and extracted ICD-10 codes and antibiotic order data. Using the urgent care and expanded ICD-10 dictionary, we classified each encounter by prescribing tier based on whether antibiotics are almost always (tier 1), sometimes (tier 2), or almost never (tier 3) indicated. For encounters with ICD-10s in multiple tiers, we chose the lowest tier. For multiple ICD-10 codes within the same tier, we chose the first extracted ICD-10 code. We calculated antibiotic prescribing rates as the proportion of encounters associated with ≥ 1 antibacterial prescription. This quality improvement project was deemed non–human subjects research by the Stanford Panel on Human Subjects in Medical Research. Results: The urgent care dictionary has 1,400 ICD-10 codes. We added 1,439 ICD-10 codes derived from primary care encounters to create the expanded ICD-10 dictionary (8.5% tier 1, 9.1% tier 2, and 82.4% tier 3) (Fig. 1). We identified 177,531 encounters; 74% had ≥ 2 associated ICD-10 codes (Fig. 2). In total, 147,085 encounters (82.9%) were classified into a tier using the urgent care dictionary. An additional 22,039 encounters were classified with the expanded dictionary (Table 1). Most added encounters were tier 3 with low 0.7% APR (Tables 1 and 3). In total, 41,473 (28.2%) encounters were classified differently depending on the ICD-10 dictionary used, most commonly changing from tier 3 to tier 2 without an increase in overall tier 2 antibiotic prescribing rate (Tables 2 and 3). Overall antibiotic prescribing rates were similar when using either the urgent care or expanded ICD-10 dictionary (Table 2). Conclusions: The expanded ICD-10 dictionary allowed for classification of more encounters in primary care; however, it did not meaningfully change antibiotic prescribing rates. Antibiotic prescribing rates were likely diluted by classifying more encounters without identifying an associated increase in antibiotic prescribing. A more sophisticated classification system may help to accommodate the diversity and volume of ICD-10 codes used in primary care.
1. Stenehjem E, et al. Clin Infect Dis 2020;70:1781–1787.
Funding: None
Disclosures: None
Outpatient hydroxychloroquine prescribing at a large academic health system during the COVID-19 pandemic
- Part of
- David R. Ha, Jamie Kuo, Phyo S. Aung, Tiffany Chang, Lana G. Witt, William Alegria, Amy Chang, Lina Meng, Stanley P. Deresinski
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 42 / Issue 3 / March 2021
- Published online by Cambridge University Press:
- 15 May 2020, pp. 377-378
- Print publication:
- March 2021
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
Simulation-based research in emergency medicine in Canada: Priorities and perspectives
- Timothy Chaplin, Brent Thoma, Andrew Petrosoniak, Kyla Caners, Tamara McColl, Chantal Forristal, Christa Dakin, Jean-Francois Deshaies, Eliane Raymond-Dufresne, Mary Fotheringham, David Ha, Nicole Holm, James Huffman, Ann-Marie Lonergan, George Mastoras, Michael O'Brien, Marie-Rose Paradis, Nicholas Sowers, Errol Stern, Andrew K. Hall
-
- Journal:
- Canadian Journal of Emergency Medicine / Volume 22 / Issue 1 / January 2020
- Published online by Cambridge University Press:
- 26 September 2019, pp. 103-111
- Print publication:
- January 2020
-
- Article
-
- You have access Access
- HTML
- Export citation
-
Objective
Simulation plays an integral role in the Canadian healthcare system with applications in quality improvement, systems development, and medical education. High-quality, simulation-based research will ensure its effective use. This study sought to summarize simulation-based research activity and its facilitators and barriers, as well as establish priorities for simulation-based research in Canadian emergency medicine (EM).
MethodsSimulation-leads from Canadian departments or divisions of EM associated with a general FRCP-EM training program surveyed and documented active EM simulation-based research at their institutions and identified the perceived facilitators and barriers. Priorities for simulation-based research were generated by simulation-leads via a second survey; these were grouped into themes and finally endorsed by consensus during an in-person meeting of simulation leads. Priority themes were also reviewed by senior simulation educators.
ResultsTwenty simulation-leads representing all 14 invited institutions participated in the study between February and May, 2018. Sixty-two active, simulation-based research projects were identified (median per institution = 4.5, IQR 4), as well as six common facilitators and five barriers. Forty-nine priorities for simulation-based research were reported and summarized into eight themes: simulation in competency-based medical education, simulation for inter-professional learning, simulation for summative assessment, simulation for continuing professional development, national curricular development, best practices in simulation-based education, simulation-based education outcomes, and simulation as an investigative methodology.
ConclusionThis study summarized simulation-based research activity in EM in Canada, identified its perceived facilitators and barriers, and built national consensus on priority research themes. This represents the first step in the development of a simulation-based research agenda specific to Canadian EM.
Cryo-EM Structure of Nipah Virus Fusion Glycoprotein in Complex with a Monoclonal Antibody Reveals Mechanism of Neutralization
- Ha V. Dang, Yee-Peng Chan, Young-Jun Park, Christopher C. Broder, David Veesler
-
- Journal:
- Microscopy and Microanalysis / Volume 25 / Issue S2 / August 2019
- Published online by Cambridge University Press:
- 05 August 2019, pp. 1328-1329
- Print publication:
- August 2019
-
- Article
-
- You have access Access
- Export citation
A Quantitative Evaluation of Microstructure by Electron Back-Scattered Diffraction Pattern Quality Variations
- Suk Hoon Kang, Hyung-Ha Jin, Jinsung Jang, Yong Seok Choi, Kyu Hwan Oh, David C. Foley, Xinghang Zhang
-
- Journal:
- Microscopy and Microanalysis / Volume 19 / Issue S5 / August 2013
- Published online by Cambridge University Press:
- 06 August 2013, pp. 83-88
- Print publication:
- August 2013
-
- Article
- Export citation
-
Band contrast (BC) is a qualitative measure of electron back-scattered diffraction (EBSD), which is derived from the intensity of the Kikuchi bands. The BC is dependent upon several factors including scanning electron microscope measurement parameters, EBSD camera setup, and the specimen itself (lattice defect and grain orientation). In this study, the effective factors for BC variations and the feasibility of using BC variations for the quantification of microstructure evolutions have been investigated. In addition, the effects of the lattice defect and the grain orientation on the BC variations are studied. Next, a shear-deformed microstructure of 316L stainless steel, which contains nanosized grains and a large portion of twin boundaries, is revealed by BC map and histogram. Recovery and recrystallization of shear-deformed 316L stainless steel are displayed by BC variations during isothermal annealing at 700 and 800°C, respectively. It is observed that the BC turns bright as the shear-deformed crystal structure is recovered or recrystallized.
Randomised, double-blind, placebo-controlled study of olanzapine in patients with bipolar I depression
- Mauricio Tohen, David P. McDonnell, Michael Case, Shigenobu Kanba, Kyooseob Ha, Yi Ru Fang, Hideaki Katagiri, Juan-Carlos Gomez
-
- Journal:
- The British Journal of Psychiatry / Volume 201 / Issue 5 / November 2012
- Published online by Cambridge University Press:
- 02 January 2018, pp. 376-382
- Print publication:
- November 2012
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
Background
Atypical antipsychotics are widely used in bipolar mania. However, the efficacy of atypical antipsychotics in bipolar depression has not been comprehensively explored.
AimsTo evaluate olanzapine monotherapy in patients with bipolar depression.
MethodPatients with bipolar depression received olanzapine (5–20mg/day, n = 343) or placebo (n = l71) for 6 weeks. The primary outcome was change from baseline to end-point in Montgomery-Åsberg Depression Rating Scale (MADRS) total score. Secondary outcomes included: Clinical Global impression - Bipolar Version (CGI-BP) scale, 17-item Hamilton Rating Scale for Depression (HRSD-17) and Young Mania Rating Scale (YMRS) scores, and the rate of response (≥50% reduction in MADRS at end-point), recovery (MADRS ≤12 for ≥4 weeks plus treatment completion) and remission (MADRS ≤8). The trial was registered with ClinicalTrials.gov (NCT00510146).
ResultsOlanzapine demonstrated: significantly greater (P<0.04) improvements on MADRS (least-squares mean change -13.82 v. -11.67), HRSD-17 and YMRS total scores and all CGI-BP subscale scores v. placebo; significantly (P≤0.05) more response and remission, but not recovery; significantly (P<0.01) greater mean increases in weight, fasting cholesterol and triglycerides; and significantly more (P<0.001) patients gained ≥7% body weight.
ConclusionsOlanzapine monotherapy appears to be efficacious in bipolar depression. Additional long-term studies are warranted to confirm these results. Safety findings were consistent with the known safety profile of olanzapine.
‘Catalytic’ doses of fructose may benefit glycaemic control without harming cardiometabolic risk factors: a small meta-analysis of randomised controlled feeding trials
- John L. Sievenpiper, Laura Chiavaroli, Russell J. de Souza, Arash Mirrahimi, Adrian I. Cozma, Vanessa Ha, D. David Wang, Matthew E. Yu, Amanda J. Carleton, Joseph Beyene, Marco Di Buono, Alexandra L. Jenkins, Lawrence A. Leiter, Thomas M. S. Wolever, Cyril W. C. Kendall, David J. A. Jenkins
-
- Journal:
- British Journal of Nutrition / Volume 108 / Issue 3 / 14 August 2012
- Published online by Cambridge University Press:
- 21 February 2012, pp. 418-423
- Print publication:
- 14 August 2012
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
Contrary to concerns that fructose may have adverse metabolic effects, there is evidence that small, ‘catalytic’ doses ( ≤ 10 g/meal) of fructose decrease the glycaemic response to high-glycaemic index meals in human subjects. To assess the longer-term effects of ‘catalytic’ doses of fructose, we undertook a meta-analysis of controlled feeding trials. We searched MEDLINE, EMBASE, CINAHL and the Cochrane Library. Analyses included all controlled feeding trials ≥ 7 d featuring ‘catalytic’ fructose doses ( ≤ 36 g/d) in isoenergetic exchange for other carbohydrates. Data were pooled by the generic inverse variance method using random-effects models and expressed as mean differences (MD) with 95 % CI. Heterogeneity was assessed by the Q statistic and quantified by I2. The Heyland Methodological Quality Score assessed study quality. A total of six feeding trials (n 118) met the eligibility criteria. ‘Catalytic’ doses of fructose significantly reduced HbA1c (MD − 0·40, 95 % CI − 0·72, − 0·08) and fasting glucose (MD − 0·25, 95 % CI − 0·44, − 0·07). This benefit was seen in the absence of adverse effects on fasting insulin, body weight, TAG or uric acid. Subgroup and sensitivity analyses showed evidence of effect modification under certain conditions. The small number of trials and their relatively short duration limit the strength of the conclusions. In conclusion, this small meta-analysis shows that ‘catalytic’ fructose doses ( ≤ 36 g/d) may improve glycaemic control without adverse effects on body weight, TAG, insulin and uric acid. There is a need for larger, longer ( ≥ 6 months) trials using ‘catalytic’ fructose to confirm these results.
Contributors
-
- By Rose Teteki Abbey, K. C. Abraham, David Tuesday Adamo, LeRoy H. Aden, Efrain Agosto, Victor Aguilan, Gillian T. W. Ahlgren, Charanjit Kaur AjitSingh, Dorothy B E A Akoto, Giuseppe Alberigo, Daniel E. Albrecht, Ruth Albrecht, Daniel O. Aleshire, Urs Altermatt, Anand Amaladass, Michael Amaladoss, James N. Amanze, Lesley G. Anderson, Thomas C. Anderson, Victor Anderson, Hope S. Antone, María Pilar Aquino, Paula Arai, Victorio Araya Guillén, S. Wesley Ariarajah, Ellen T. Armour, Brett Gregory Armstrong, Atsuhiro Asano, Naim Stifan Ateek, Mahmoud Ayoub, John Alembillah Azumah, Mercedes L. García Bachmann, Irena Backus, J. Wayne Baker, Mieke Bal, Lewis V. Baldwin, William Barbieri, António Barbosa da Silva, David Basinger, Bolaji Olukemi Bateye, Oswald Bayer, Daniel H. Bays, Rosalie Beck, Nancy Elizabeth Bedford, Guy-Thomas Bedouelle, Chorbishop Seely Beggiani, Wolfgang Behringer, Christopher M. Bellitto, Byard Bennett, Harold V. Bennett, Teresa Berger, Miguel A. Bernad, Henley Bernard, Alan E. Bernstein, Jon L. Berquist, Johannes Beutler, Ana María Bidegain, Matthew P. Binkewicz, Jennifer Bird, Joseph Blenkinsopp, Dmytro Bondarenko, Paulo Bonfatti, Riet en Pim Bons-Storm, Jessica A. Boon, Marcus J. Borg, Mark Bosco, Peter C. Bouteneff, François Bovon, William D. Bowman, Paul S. Boyer, David Brakke, Richard E. Brantley, Marcus Braybrooke, Ian Breward, Ênio José da Costa Brito, Jewel Spears Brooker, Johannes Brosseder, Nicholas Canfield Read Brown, Robert F. Brown, Pamela K. Brubaker, Walter Brueggemann, Bishop Colin O. Buchanan, Stanley M. Burgess, Amy Nelson Burnett, J. Patout Burns, David B. Burrell, David Buttrick, James P. Byrd, Lavinia Byrne, Gerado Caetano, Marcos Caldas, Alkiviadis Calivas, William J. Callahan, Salvatore Calomino, Euan K. Cameron, William S. Campbell, Marcelo Ayres Camurça, Daniel F. Caner, Paul E. Capetz, Carlos F. Cardoza-Orlandi, Patrick W. Carey, Barbara Carvill, Hal Cauthron, Subhadra Mitra Channa, Mark D. Chapman, James H. Charlesworth, Kenneth R. Chase, Chen Zemin, Luciano Chianeque, Philip Chia Phin Yin, Francisca H. Chimhanda, Daniel Chiquete, John T. Chirban, Soobin Choi, Robert Choquette, Mita Choudhury, Gerald Christianson, John Chryssavgis, Sejong Chun, Esther Chung-Kim, Charles M. A. Clark, Elizabeth A. Clark, Sathianathan Clarke, Fred Cloud, John B. Cobb, W. Owen Cole, John A Coleman, John J. Collins, Sylvia Collins-Mayo, Paul K. Conkin, Beth A. Conklin, Sean Connolly, Demetrios J. Constantelos, Michael A. Conway, Paula M. Cooey, Austin Cooper, Michael L. Cooper-White, Pamela Cooper-White, L. William Countryman, Sérgio Coutinho, Pamela Couture, Shannon Craigo-Snell, James L. Crenshaw, David Crowner, Humberto Horacio Cucchetti, Lawrence S. Cunningham, Elizabeth Mason Currier, Emmanuel Cutrone, Mary L. Daniel, David D. Daniels, Robert Darden, Rolf Darge, Isaiah Dau, Jeffry C. Davis, Jane Dawson, Valentin Dedji, John W. de Gruchy, Paul DeHart, Wendy J. Deichmann Edwards, Miguel A. De La Torre, George E. Demacopoulos, Thomas de Mayo, Leah DeVun, Beatriz de Vasconcellos Dias, Dennis C. Dickerson, John M. Dillon, Luis Miguel Donatello, Igor Dorfmann-Lazarev, Susanna Drake, Jonathan A. Draper, N. Dreher Martin, Otto Dreydoppel, Angelyn Dries, A. J. Droge, Francis X. D'Sa, Marilyn Dunn, Nicole Wilkinson Duran, Rifaat Ebied, Mark J. Edwards, William H. Edwards, Leonard H. Ehrlich, Nancy L. Eiesland, Martin Elbel, J. Harold Ellens, Stephen Ellingson, Marvin M. Ellison, Robert Ellsberg, Jean Bethke Elshtain, Eldon Jay Epp, Peter C. Erb, Tassilo Erhardt, Maria Erling, Noel Leo Erskine, Gillian R. Evans, Virginia Fabella, Michael A. Fahey, Edward Farley, Margaret A. Farley, Wendy Farley, Robert Fastiggi, Seena Fazel, Duncan S. Ferguson, Helwar Figueroa, Paul Corby Finney, Kyriaki Karidoyanes FitzGerald, Thomas E. FitzGerald, John R. Fitzmier, Marie Therese Flanagan, Sabina Flanagan, Claude Flipo, Ronald B. Flowers, Carole Fontaine, David Ford, Mary Ford, Stephanie A. Ford, Jim Forest, William Franke, Robert M. Franklin, Ruth Franzén, Edward H. Friedman, Samuel Frouisou, Lorelei F. Fuchs, Jojo M. Fung, Inger Furseth, Richard R. Gaillardetz, Brandon Gallaher, China Galland, Mark Galli, Ismael García, Tharscisse Gatwa, Jean-Marie Gaudeul, Luis María Gavilanes del Castillo, Pavel L. Gavrilyuk, Volney P. Gay, Metropolitan Athanasios Geevargis, Kondothra M. George, Mary Gerhart, Simon Gikandi, Maurice Gilbert, Michael J. Gillgannon, Verónica Giménez Beliveau, Terryl Givens, Beth Glazier-McDonald, Philip Gleason, Menghun Goh, Brian Golding, Bishop Hilario M. Gomez, Michelle A. Gonzalez, Donald K. Gorrell, Roy Gottfried, Tamara Grdzelidze, Joel B. Green, Niels Henrik Gregersen, Cristina Grenholm, Herbert Griffiths, Eric W. Gritsch, Erich S. Gruen, Christoffer H. Grundmann, Paul H. Gundani, Jon P. Gunnemann, Petre Guran, Vidar L. Haanes, Jeremiah M. Hackett, Getatchew Haile, Douglas John Hall, Nicholas Hammond, Daphne Hampson, Jehu J. Hanciles, Barry Hankins, Jennifer Haraguchi, Stanley S. Harakas, Anthony John Harding, Conrad L. Harkins, J. William Harmless, Marjory Harper, Amir Harrak, Joel F. Harrington, Mark W. Harris, Susan Ashbrook Harvey, Van A. Harvey, R. Chris Hassel, Jione Havea, Daniel Hawk, Diana L. Hayes, Leslie Hayes, Priscilla Hayner, S. Mark Heim, Simo Heininen, Richard P. Heitzenrater, Eila Helander, David Hempton, Scott H. Hendrix, Jan-Olav Henriksen, Gina Hens-Piazza, Carter Heyward, Nicholas J. Higham, David Hilliard, Norman A. Hjelm, Peter C. Hodgson, Arthur Holder, M. Jan Holton, Dwight N. Hopkins, Ronnie Po-chia Hsia, Po-Ho Huang, James Hudnut-Beumler, Jennifer S. Hughes, Leonard M. Hummel, Mary E. Hunt, Laennec Hurbon, Mark Hutchinson, Susan E. Hylen, Mary Beth Ingham, H. Larry Ingle, Dale T. Irvin, Jon Isaak, Paul John Isaak, Ada María Isasi-Díaz, Hans Raun Iversen, Margaret C. Jacob, Arthur James, Maria Jansdotter-Samuelsson, David Jasper, Werner G. Jeanrond, Renée Jeffery, David Lyle Jeffrey, Theodore W. Jennings, David H. Jensen, Robin Margaret Jensen, David Jobling, Dale A. Johnson, Elizabeth A. Johnson, Maxwell E. Johnson, Sarah Johnson, Mark D. Johnston, F. Stanley Jones, James William Jones, John R. Jones, Alissa Jones Nelson, Inge Jonsson, Jan Joosten, Elizabeth Judd, Mulambya Peggy Kabonde, Robert Kaggwa, Sylvester Kahakwa, Isaac Kalimi, Ogbu U. Kalu, Eunice Kamaara, Wayne C. Kannaday, Musimbi Kanyoro, Veli-Matti Kärkkäinen, Frank Kaufmann, Léon Nguapitshi Kayongo, Richard Kearney, Alice A. Keefe, Ralph Keen, Catherine Keller, Anthony J. Kelly, Karen Kennelly, Kathi Lynn Kern, Fergus Kerr, Edward Kessler, George Kilcourse, Heup Young Kim, Kim Sung-Hae, Kim Yong-Bock, Kim Yung Suk, Richard King, Thomas M. King, Robert M. Kingdon, Ross Kinsler, Hans G. Kippenberg, Cheryl A. Kirk-Duggan, Clifton Kirkpatrick, Leonid Kishkovsky, Nadieszda Kizenko, Jeffrey Klaiber, Hans-Josef Klauck, Sidney Knight, Samuel Kobia, Robert Kolb, Karla Ann Koll, Heikki Kotila, Donald Kraybill, Philip D. W. Krey, Yves Krumenacker, Jeffrey Kah-Jin Kuan, Simanga R. Kumalo, Peter Kuzmic, Simon Shui-Man Kwan, Kwok Pui-lan, André LaCocque, Stephen E. Lahey, John Tsz Pang Lai, Emiel Lamberts, Armando Lampe, Craig Lampe, Beverly J. Lanzetta, Eve LaPlante, Lizette Larson-Miller, Ariel Bybee Laughton, Leonard Lawlor, Bentley Layton, Robin A. Leaver, Karen Lebacqz, Archie Chi Chung Lee, Marilyn J. Legge, Hervé LeGrand, D. L. LeMahieu, Raymond Lemieux, Bill J. Leonard, Ellen M. Leonard, Outi Leppä, Jean Lesaulnier, Nantawan Boonprasat Lewis, Henrietta Leyser, Alexei Lidov, Bernard Lightman, Paul Chang-Ha Lim, Carter Lindberg, Mark R. Lindsay, James R. Linville, James C. Livingston, Ann Loades, David Loades, Jean-Claude Loba-Mkole, Lo Lung Kwong, Wati Longchar, Eleazar López, David W. Lotz, Andrew Louth, Robin W. Lovin, William Luis, Frank D. Macchia, Diarmaid N. J. MacCulloch, Kirk R. MacGregor, Marjory A. MacLean, Donald MacLeod, Tomas S. Maddela, Inge Mager, Laurenti Magesa, David G. Maillu, Fortunato Mallimaci, Philip Mamalakis, Kä Mana, Ukachukwu Chris Manus, Herbert Robinson Marbury, Reuel Norman Marigza, Jacqueline Mariña, Antti Marjanen, Luiz C. L. Marques, Madipoane Masenya (ngwan'a Mphahlele), Caleb J. D. Maskell, Steve Mason, Thomas Massaro, Fernando Matamoros Ponce, András Máté-Tóth, Odair Pedroso Mateus, Dinis Matsolo, Fumitaka Matsuoka, John D'Arcy May, Yelena Mazour-Matusevich, Theodore Mbazumutima, John S. McClure, Christian McConnell, Lee Martin McDonald, Gary B. McGee, Thomas McGowan, Alister E. McGrath, Richard J. McGregor, John A. McGuckin, Maud Burnett McInerney, Elsie Anne McKee, Mary B. McKinley, James F. McMillan, Ernan McMullin, Kathleen E. McVey, M. Douglas Meeks, Monica Jyotsna Melanchthon, Ilie Melniciuc-Puica, Everett Mendoza, Raymond A. Mentzer, William W. Menzies, Ina Merdjanova, Franziska Metzger, Constant J. Mews, Marvin Meyer, Carol Meyers, Vasile Mihoc, Gunner Bjerg Mikkelsen, Maria Inêz de Castro Millen, Clyde Lee Miller, Bonnie J. Miller-McLemore, Alexander Mirkovic, Paul Misner, Nozomu Miyahira, R. W. L. Moberly, Gerald Moede, Aloo Osotsi Mojola, Sunanda Mongia, Rebeca Montemayor, James Moore, Roger E. Moore, Craig E. Morrison O.Carm, Jeffry H. Morrison, Keith Morrison, Wilson J. Moses, Tefetso Henry Mothibe, Mokgethi Motlhabi, Fulata Moyo, Henry Mugabe, Jesse Ndwiga Kanyua Mugambi, Peggy Mulambya-Kabonde, Robert Bruce Mullin, Pamela Mullins Reaves, Saskia Murk Jansen, Heleen L. Murre-Van den Berg, Augustine Musopole, Isaac M. T. Mwase, Philomena Mwaura, Cecilia Nahnfeldt, Anne Nasimiyu Wasike, Carmiña Navia Velasco, Thulani Ndlazi, Alexander Negrov, James B. Nelson, David G. Newcombe, Carol Newsom, Helen J. Nicholson, George W. E. Nickelsburg, Tatyana Nikolskaya, Damayanthi M. A. Niles, Bertil Nilsson, Nyambura Njoroge, Fidelis Nkomazana, Mary Beth Norton, Christian Nottmeier, Sonene Nyawo, Anthère Nzabatsinda, Edward T. Oakes, Gerald O'Collins, Daniel O'Connell, David W. Odell-Scott, Mercy Amba Oduyoye, Kathleen O'Grady, Oyeronke Olajubu, Thomas O'Loughlin, Dennis T. Olson, J. Steven O'Malley, Cephas N. Omenyo, Muriel Orevillo-Montenegro, César Augusto Ornellas Ramos, Agbonkhianmeghe E. Orobator, Kenan B. Osborne, Carolyn Osiek, Javier Otaola Montagne, Douglas F. Ottati, Anna May Say Pa, Irina Paert, Jerry G. Pankhurst, Aristotle Papanikolaou, Samuele F. Pardini, Stefano Parenti, Peter Paris, Sung Bae Park, Cristián G. Parker, Raquel Pastor, Joseph Pathrapankal, Daniel Patte, W. Brown Patterson, Clive Pearson, Keith F. Pecklers, Nancy Cardoso Pereira, David Horace Perkins, Pheme Perkins, Edward N. Peters, Rebecca Todd Peters, Bishop Yeznik Petrossian, Raymond Pfister, Peter C. Phan, Isabel Apawo Phiri, William S. F. Pickering, Derrick G. Pitard, William Elvis Plata, Zlatko Plese, John Plummer, James Newton Poling, Ronald Popivchak, Andrew Porter, Ute Possekel, James M. Powell, Enos Das Pradhan, Devadasan Premnath, Jaime Adrían Prieto Valladares, Anne Primavesi, Randall Prior, María Alicia Puente Lutteroth, Eduardo Guzmão Quadros, Albert Rabil, Laurent William Ramambason, Apolonio M. Ranche, Vololona Randriamanantena Andriamitandrina, Lawrence R. Rast, Paul L. Redditt, Adele Reinhartz, Rolf Rendtorff, Pål Repstad, James N. Rhodes, John K. Riches, Joerg Rieger, Sharon H. Ringe, Sandra Rios, Tyler Roberts, David M. Robinson, James M. Robinson, Joanne Maguire Robinson, Richard A. H. Robinson, Roy R. Robson, Jack B. Rogers, Maria Roginska, Sidney Rooy, Rev. Garnett Roper, Maria José Fontelas Rosado-Nunes, Andrew C. Ross, Stefan Rossbach, François Rossier, John D. Roth, John K. Roth, Phillip Rothwell, Richard E. Rubenstein, Rosemary Radford Ruether, Markku Ruotsila, John E. Rybolt, Risto Saarinen, John Saillant, Juan Sanchez, Wagner Lopes Sanchez, Hugo N. Santos, Gerhard Sauter, Gloria L. Schaab, Sandra M. Schneiders, Quentin J. Schultze, Fernando F. Segovia, Turid Karlsen Seim, Carsten Selch Jensen, Alan P. F. Sell, Frank C. Senn, Kent Davis Sensenig, Damían Setton, Bal Krishna Sharma, Carolyn J. Sharp, Thomas Sheehan, N. Gerald Shenk, Christian Sheppard, Charles Sherlock, Tabona Shoko, Walter B. Shurden, Marguerite Shuster, B. Mark Sietsema, Batara Sihombing, Neil Silberman, Clodomiro Siller, Samuel Silva-Gotay, Heikki Silvet, John K. Simmons, Hagith Sivan, James C. Skedros, Abraham Smith, Ashley A. Smith, Ted A. Smith, Daud Soesilo, Pia Søltoft, Choan-Seng (C. S.) Song, Kathryn Spink, Bryan Spinks, Eric O. Springsted, Nicolas Standaert, Brian Stanley, Glen H. Stassen, Karel Steenbrink, Stephen J. Stein, Andrea Sterk, Gregory E. Sterling, Columba Stewart, Jacques Stewart, Robert B. Stewart, Cynthia Stokes Brown, Ken Stone, Anne Stott, Elizabeth Stuart, Monya Stubbs, Marjorie Hewitt Suchocki, David Kwang-sun Suh, Scott W. Sunquist, Keith Suter, Douglas Sweeney, Charles H. Talbert, Shawqi N. Talia, Elsa Tamez, Joseph B. Tamney, Jonathan Y. Tan, Yak-Hwee Tan, Kathryn Tanner, Feiya Tao, Elizabeth S. Tapia, Aquiline Tarimo, Claire Taylor, Mark Lewis Taylor, Bishop Abba Samuel Wolde Tekestebirhan, Eugene TeSelle, M. Thomas Thangaraj, David R. Thomas, Andrew Thornley, Scott Thumma, Marcelo Timotheo da Costa, George E. “Tink” Tinker, Ola Tjørhom, Karen Jo Torjesen, Iain R. Torrance, Fernando Torres-Londoño, Archbishop Demetrios [Trakatellis], Marit Trelstad, Christine Trevett, Phyllis Trible, Johannes Tromp, Paul Turner, Robert G. Tuttle, Archbishop Desmond Tutu, Peter Tyler, Anders Tyrberg, Justin Ukpong, Javier Ulloa, Camillus Umoh, Kristi Upson-Saia, Martina Urban, Monica Uribe, Elochukwu Eugene Uzukwu, Richard Vaggione, Gabriel Vahanian, Paul Valliere, T. J. Van Bavel, Steven Vanderputten, Peter Van der Veer, Huub Van de Sandt, Louis Van Tongeren, Luke A. Veronis, Noel Villalba, Ramón Vinke, Tim Vivian, David Voas, Elena Volkova, Katharina von Kellenbach, Elina Vuola, Timothy Wadkins, Elaine M. Wainwright, Randi Jones Walker, Dewey D. Wallace, Jerry Walls, Michael J. Walsh, Philip Walters, Janet Walton, Jonathan L. Walton, Wang Xiaochao, Patricia A. Ward, David Harrington Watt, Herold D. Weiss, Laurence L. Welborn, Sharon D. Welch, Timothy Wengert, Traci C. West, Merold Westphal, David Wetherell, Barbara Wheeler, Carolinne White, Jean-Paul Wiest, Frans Wijsen, Terry L. Wilder, Felix Wilfred, Rebecca Wilkin, Daniel H. Williams, D. Newell Williams, Michael A. Williams, Vincent L. Wimbush, Gabriele Winkler, Anders Winroth, Lauri Emílio Wirth, James A. Wiseman, Ebba Witt-Brattström, Teofil Wojciechowski, John Wolffe, Kenman L. Wong, Wong Wai Ching, Linda Woodhead, Wendy M. Wright, Rose Wu, Keith E. Yandell, Gale A. Yee, Viktor Yelensky, Yeo Khiok-Khng, Gustav K. K. Yeung, Angela Yiu, Amos Yong, Yong Ting Jin, You Bin, Youhanna Nessim Youssef, Eliana Yunes, Robert Michael Zaller, Valarie H. Ziegler, Barbara Brown Zikmund, Joyce Ann Zimmerman, Aurora Zlotnik, Zhuo Xinping
- Edited by Daniel Patte, Vanderbilt University, Tennessee
-
- Book:
- The Cambridge Dictionary of Christianity
- Published online:
- 05 August 2012
- Print publication:
- 20 September 2010, pp xi-xliv
-
- Chapter
- Export citation
Personality and Political Attitudes: Relationships across Issue Domains and Political Contexts
- ALAN S. GERBER, GREGORY A. HUBER, DAVID DOHERTY, CONOR M. DOWLING, SHANG E. HA
-
- Journal:
- American Political Science Review / Volume 104 / Issue 1 / February 2010
- Published online by Cambridge University Press:
- 18 March 2010, pp. 111-133
- Print publication:
- February 2010
-
- Article
- Export citation
-
Previous research on personality traits and political attitudes has largely focused on the direct relationships between traits and ideological self-placement. There are theoretical reasons, however, to suspect that the relationships between personality traits and political attitudes (1) vary across issue domains and (2) depend on contextual factors that affect the meaning of political stimuli. In this study, we provide an explicit theoretical framework for formulating hypotheses about these differential effects. We then leverage the power of an unusually large national survey of registered voters to examine how the relationships between Big Five personality traits and political attitudes differ across issue domains and social contexts (as defined by racial groups). We confirm some important previous findings regarding personality and political ideology, find clear evidence that Big Five traits affect economic and social attitudes differently, show that the effect of Big Five traits is often as large as that of education or income in predicting ideology, and demonstrate that the relationships between Big Five traits and ideology vary substantially between white and black respondents.
Molecular Beam Epitaxy Growth of High Mobility Compound Semiconductor Devices for Integration with Si CMOS
- Dmitri Lubyshev, Joel M. Fastenau, Ying Wu, Andrew Synder, Amy W. K. Liu, Mayank T. Bulsara, Eugene A. Fitzgerald, Miguel Urteaga, Wonill Ha, Joshua Bergman, M. J. Choe, Bobby Brar, William E. Hoke, Jeffrey R. LaRoche, Abbas Torabi, Thomas E. Kazior, David Smith, David Clark, Robin F. Thompson, Charlotte Drazek, Nicolas Daval, Lamine Benaissa, Emmanuel Augendre
-
- Journal:
- MRS Online Proceedings Library Archive / Volume 1194 / 2009
- Published online by Cambridge University Press:
- 31 January 2011, 1194-A09-01
- Print publication:
- 2009
-
- Article
- Export citation
-
We report on a direct epitaxial growth approach for the heterogeneous integration of high speed III-V devices with Si CMOS logic on a common Si substrate. InP-based heterojunction bipolar transistor (HBTs) structures were successfully grown on patterned Si-on-Lattice-Engineered-Substrate (SOLES) substrates using molecular beam epitaxy. DC and RF performance similar to those grown on lattice-matched InP were achieved in growth windows as small as 15×15μm2. This truly planar approach allows tight device placement with InP-HBTs to Si CMOS transistors separation as small as 2.5 μm, and the use of standard wafer level multilayer interconnects. A high speed, low power dissipation differential amplifier was designed and fabricated, demonstrating the feasibility of using this approach for high performance mixed signal circuits such as ADCs and DACs.
Electrically Modulated Drug Delivery using Nanoporous Electrodes
- David B. Robinson, Shaun D. Gittard, C.-A. Max Wu, Cindy M. Ha, Roger J. Narayan
-
- Journal:
- MRS Online Proceedings Library Archive / Volume 1239 / 2009
- Published online by Cambridge University Press:
- 31 January 2011, 1239-VV08-03
- Print publication:
- 2009
-
- Article
- Export citation
-
Nanoporous electrodes, such as those made from carbon or gold, can capture and release ionic analytes at concentrations near 1 mole per liter of pore volume through capacitive charging or electrochemically reversible adsorption. In vitro studies suggest that this phenomenon can be the basis for a noninvasive, precise, and programmable drug delivery method. It would eliminate the need for bulk fluid delivery to target tissue and require only a thin electrical connection, minimizing pain and tissue disruption. We have designed effective gold electrode assemblies and observed the depletion and release phenomena using electrochemical methods and charged dyes.
Direct Growth of III-V Devices on Silicon
- Katherine Herrick, Thomas Kazior, Amy Liu, Dmitri I. Loubychev, Joel M. Fastenau, Miguel Urteaga, Eugene A. Fitzgerald, Mayank T. Bulsara, David Clark, Berinder Brar, Wonill Ha, Joshua Bergman, Nicolas Daval, Jeffrey LaRoche
-
- Journal:
- MRS Online Proceedings Library Archive / Volume 1068 / 2008
- Published online by Cambridge University Press:
- 01 February 2011, 1068-C02-01
- Print publication:
- 2008
-
- Article
- Export citation
-
Our direct growth approach of integrating compound semiconductors (CS) and silicon CMOS is based on a unique silicon template wafer with an embedded CS template layer of Germanium (Ge). It enables selective placement of CS devices in arbitrary locations on a Silicon CMOS wafer for simple, high yield, monolithic integration and optimal circuit performance. HBTs demonstrate a peak current gain cutoff frequency ft of 170GHz at a nominal collector current density of 2mA/μm2. To the best of our knowledge this represents the first demonstration of an InP-based HBT fabricated on a silicon wafer.
behavioral aspects of lesch–nyhan disease and its variants
- david j schretlen, julianna ward, stephen m meyer, jonathan yun, juan g puig, william l nyhan, ha jinnah, james c harris
-
- Journal:
- Developmental Medicine and Child Neurology / Volume 47 / Issue 10 / October 2005
- Published online by Cambridge University Press:
- 12 September 2005, pp. 673-677
- Print publication:
- October 2005
-
- Article
- Export citation
-
self-injury is a defining feature of lesch–nyhan disease (lnd) but does not occur in the less severely affected lesch–nyhan variants (lnv). the aim of this study was to quantify behavioral and emotional abnormalities in lnd and lnv. thirty-nine informants rated 22 patients with lnd (21 males, 1 female), 11 males with lnv, and 11 healthy controls (hc; 10 males, 1 female) using two well-validated rating scales. the age of patients with lnd ranged from 12 years 7 months to 38 years 3 months (mean 22y 11mo; sd 7y 8mo), whereas the age range of those with lnv was 12 years 9 months to 65 years (mean 30y 7mo; sd 15y 2mo), and the healthy controls were aged 12 years 4 months to 31 years 3 months (mean 17y 10mo; sd 5y 7mo). behavioral ratings were based on the child behavior checklist and the american association on mental retardation's adaptive behavior scale – residential and community, 2nd edition. statistical analyses revealed that patients with lnd showed severe self-injury together with problematic aggression, anxious-depressed symptoms, distractibility, motor stereotypes, and disturbing interpersonal behaviors. patients with lnv were rated as being intermediate between the hc and lnd groups on all behavior scales. although the lnv group did not differ from hcs on most scales, their reported attention problems were as severe as those found in lnd. we conclude that self-injurious and aggressive behaviors are nearly universal and that other behavioral abnormalities are common in lnd. although patients with lnv typically do not self-injure or display severe aggression, attention problems are common and a few patients demonstrate other behavioral anomalies.

















